Services We Offer
We’re hereby pleased to tell you that we’re the ones you were trying to find Sapphire is a leading provider of Revenue Cycle Management and Claim Adjustment Services .Sapphire brings to you the best available and undeniable services when it comes to the topic of healthcare financing, physician credentialing and all other related topics. So don’t stay stuck between your health practice and credentialing management and let our expertise provide you the maximum profit.
Regardless of the size of your customers, we have the expertise and resources to increase your cash flow, reduce your operational costs, and much more that you’ll be benefited with.
We strive to make life better for providers, staff and patients.
 Physician Credentialing Services
Physician Credentialing Services
Physicians and healthcare practitioners trying to bill an insurance company and receive reimbursement for services are all invited here.
As we all know Credentialing or enrolling with government and commercial payers is challenging any way you slice it, but we’re here to eliminate all the stress and let you rest and also increase the efficiency. We take care of everything from start to finish and keep you from spinning your wheels on the telephone for 4 hours a day.
Physicians and other healthcare practitioners who wish to bill an insurance company and receive reimbursement for services are invited to contact us as an in-network provider must undergo a process of credentialing in which the insurance company verifies the providers education, training, experience, and competency. Our team of experts understand the insurance companies, and as former practice managers, we also understand what these insurance contracts mean to you.
In a busy practice, we understand how difficult it can be to manage all of your current duties and also try to keep up with populating, maintaining, submitting, and tracking credentialing applications for physicians and allied professionals.
So contact us and instead of taking all these headaches You’ll be able to:-
- Concentrate time on patient care instead of credentialing headaches.
- Shift the paperwork and errors to our desks.
- Relieve valuable staff of the headaching credentialing.
- Gain access to preferred insurance networks quickly and efficiently with our specialized credentialing services.
As you are joining us ,So you don’t have to worry about credentialing, and waste your valuable time and energy which instead can be focused on caring for your patients and growing the practice.
 Insurance Eligibility Verification
Insurance Eligibility Verification
Insurance eligibility verification is the most important step in the medical billing process. So getting the claims accepted, on the first submission is always and will ever remain our basic criterion.
Are you or your staff tired of waiting on the phone or website to verify patients’ insurance eligibility? Being able to verify a patient’s eligibility and benefits information in a timely manner is critical. To do this consistently, you need support that is easy, efficient and cost effective. Sapphire simplifies this process for you.
Research confirms that most of the claims are denied or delayed due to inadequate or incorrect coverage information provided by the patients during visits and current coverage information not updated by the office / hospital staff and this lack of or improper insurance eligibility verification directly impacts the reimbursements.
But don’t you worry as we’re here to save you from all those problems and get you the maximum possible reimbursements.
Sapphire’s insurance eligibility and benefits verification service obtains all pertinent information required – not only coverage confirmation but also tells you aboutbut what kind of coverage the patient has, what their deductible is, and how much has been applied. Having all necessary information generates more revenue and reduces administrative costs.
 Practice management and Consulting
Practice management and Consulting
It can be difficult at times to both care for patients and manage the business side of your practice. Our practice management services provide help in areas of need when assistance is required, from everyday tasks like office workflow improvements and operational procedures to managing your revenue cycle.
Practice management is the most flexible aspect of the services that Sapphire provides because each scope of services is customized to the specific business situation and requirements of each medical practice. It is also the highest level of service provided by Sapphire.
Our team provides the insight, expertise and tools you need to strategically manage reimbursement and evaluate periodic organization and expansion opportunities.
Sapphire helps practices evaluate and negotiate managed care agreements, giving you the insight needed to help win the terms and rates your practice deserves. Sapphire can help you gain insight into managed care agreements, including contract negotiation support and advice on financial, strategic and administrative aspects of payer agreements.
 Medical Billing and Coding
Medical Billing and Coding
Being our customer, your medical facility can get access to quality medical coding and billing, while reducing your current operating costs. Our medical billing and coding solutions will meet all your needs, from following up on pending medical claims, to getting reasons for the denied claims, locating and initiating collections. Our specialists understand the revenue cycle, ensure that the coding and processing is done in a timely manner, and provide the follow-up on the claims as well.
We have best practices to help with the billing collections and reduce the time to get you paid. We have the latest technology at our hand merged with a customer service approach that makes it easy to collect when it is necessary.
So don’t let your patient bills get bounced, slowing down and creating a hindrance in your work stream you have coming in to your practice. We provide the quality services you need for coding and billing so you can get your finances back on track and streamline the operations of your office.
Medical coding is the main factor that impacts your practice. Without expertise, you are going to expose yourself to risk. With our support, you can get lesser denials, and greater revenue.
 Revenue Cycle Management
Revenue Cycle Management
Sapphire’s team of experts helps you with your Revenue Cycle Management (“RCM”) and performs every required activities like authorizations, benefit verification, data abstraction, etc., and rotates the maximized output to your profit and always thrive to improve operational efficiencies & customer retention & reduce expenses &improve and recover more receivables.
Sapphire offers a comprehensive revenue cycle management solution to improve your health financially and allow you to focus on your clinical practice.
Some Insights of Sapphire’s full service RCM 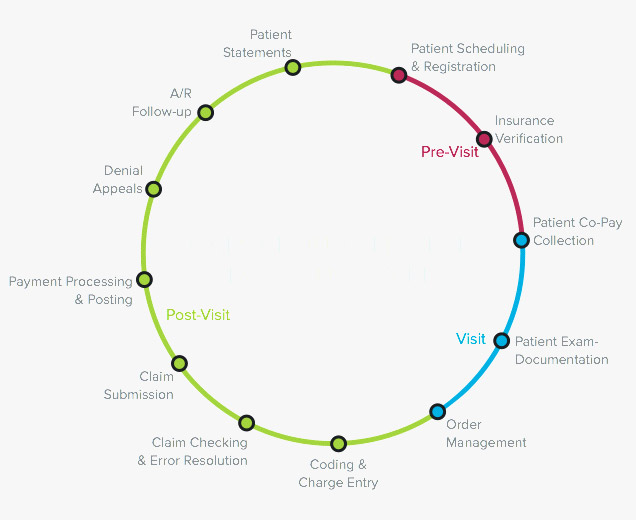
- Fee Schedule Review and Analysis
- Eligibility and Benefit Verification (?)
- Provider Credentialing and Enrollment INCLUDED
- Electronic and Paper Claims Submission
- Account Receivables Management
- Secondary Insurance Billing
- Incoming patient calls
- Old Account Receivables Recovery
- Authorization Request and Tracking (?)
- Charge Entry – All Specialties Posting of Insurance and Patient Payments
- Extensive Insurance Follow Up
- Patient Statement Processing and Mailing
- Denial Review and Management
- Appeal of Denied or Low Paid Claims
Contact us today to find out more about our services and solutions that are available to you. As your partner, we want to show you how your business can be more efficient today.





